Thyroiditis is inflammation of the thyroid gland. Subacute thyroiditis (or subacute granulomatous thyroiditis) and infectious thyroiditis (or suppurative thyroiditis) can manifest as an acute or subacute illness.
On the other hand, painless ( or silent thyroiditis) and fibrous (Reidels thyroiditis) can present only with thyroid dysfunction.
How Subacute Thyroiditis can present?

Subacute thyroiditis is manifested by neck pain, tender goiter, and elevated Thyroid hormones (T3 and T4).
Inflammation causes the release of already formed thyroid hormones, so patients present initially with a hyperthyroid state.
When the inflammation is severe enough that it destroys most of the thyroid gland, the patient may go into a transient or in the very severe cases a permanent state of hypothyroidism. These patients usually require lifelong thyroxine.
Variants of Subacute Thyroiditis:
There are three different variants of subacute thyroiditis. These include:
Subacute granulomatous thyroiditis – Also known as subacute painful or de Quervain thyroiditis (see the image below)
Subacute lymphocytic thyroiditis – Also known as subacute painless thyroiditis
Subacute postpartum thyroiditis
What Causes Subacute Thyroiditis?
It is presumed to be caused by a viral infection or postviral inflammatory process, because many patients have a history of an upper respiratory infection preceding the onset of thyroiditis, and clusters of cases have occurred in association with epidemics of Coxsackievirus or other viral infections. There is a strong association with HLA-B35.
Other causes include drugs and postpartum thyroiditis. Postpartum thyroiditis occurs in females within one year after parturition or a miscarriage. The disease is self-limited and it may at times be very difficult to differentiate postpartum thyroiditis from graves disease.
Investigations in subacute thyroiditis:
Patients may have raised inflammatory markers. ESR may be above 100 mm in the first hour in some cases. White cell counts may rise.
Thyroid function tests may be suggestive of a hyperthyroid state. S.TSH will be low, T4 and T3 will be high.

Thyroid scan will be cold i.e. less than 1% of the radiotracer material will be taken up by the thyroid gland.
Thyroid imaging includes a thyroid ultrasound, doppler of the thyroid gland, CT and MR of the thyroid gland.
How to treat Subacute Thyroiditis?
Subacute thyroiditis is a self-resolving disease. treatment is symptomatic, however anti-thyroid drugs have no role as only the preformed thyroxine is released from the thyroid gland.
Supportive treatment includes nonsteroidal anti-inflammatory drugs, beta-blockers, steroids, hydration and monitoring of thyroid functions.
How does Infectious Thyroiditis Present?
Infection in the thyroid gland can be caused by a hematogenous spread or from a local ENT disease (via a fistula from the piriform sinus adjacent to the larynx). It may be acute or chronic.
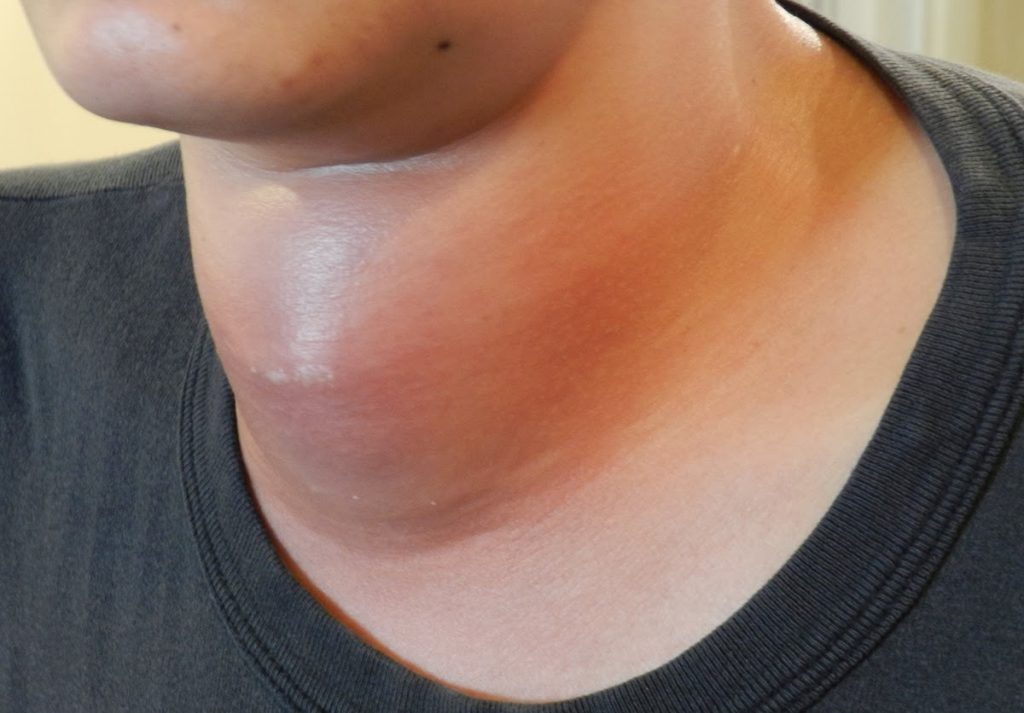
Acute infectious thyroiditis usually is usually caused by gram-negative organisms and staphylococci. Chronic infections include tuberculosis, fungal and Pneumocystis jirovecii pneumonia(in immunocompromised patients).
Patients may present with a high-grade fever and neck pain usually localized to one lobe. Thyroid ultrasound and FNAC can differentiate between subacute thyroiditis and infectious thyroiditis. Treatment consists of intravenous antibiotics and drainage of the abscess in some patients.
What are other forms of thyroiditis?
Radiation thyroiditis develops in patients 5 to 10 days after treatment with a radioactive Iodine (for Graves or other forms of toxic goiter). The condition is associated with a transient hyperthyroid state.
Trauma, vigorous palpation (palpation thyroiditis), neck surgery, and thyroid manipulation during biopsy or surgery of the parathyroid gland can manifest with neck pain and a transient state of hyperthyroidism.
Thyroiditis can be painless as well.
Causes of silent or painless thyroiditis include silent (lymphocytic thyroiditis), postpartum thyroiditis, drug-induced thyroiditis, and fibrous thyroiditis.
Drugs causing thyroiditis include Interferon-alfa, Interleukin-2, Denileukin diftitox, Amiodarone, Lithium and Kinase inhibitors.
Briefly about Fibrous thyroiditis:
Fibrous thyroiditis, also known as Riedel’s thyroiditis or invasive thyroiditis, is characterized by extensive fibrosis and macrophage and eosinophil infiltration of the thyroid gland that extends into adjacent tissues.
It is probably a primary fibrosing disorder and has been reported in patients who also had mediastinal and retroperitoneal fibrosis.
Affected patients have neck discomfort or tightness, sometimes dysphagia or hoarseness, and a diffuse, although occasionally asymmetric, goiter that is very hard, fixed, and often not clearly separable from the adjacent tissues.
Most patients are euthyroid, but a few are hypothyroid, and serum antithyroid antibody concentrations are often high. The diagnosis is established by a thyroid biopsy.
Patients should be evaluated for evidence of systemic fibrosis in other areas, such as mediastinum and retroperitoneal areas.