Meningitis is inflammation of the membranes covering the brain called meninges. It usually follows a bloodstream infection, pneumonia, pelvic and urinary tract infection, and upper respiratory tract infection.
Meningitis may be caused by bacterial, fungal, tuberculous, or viral infections. The most common bacteria causing meningitis in adults is streptococcus pneumonia. In newborns, E.coli is the most common cause of meningitis.
What are the symptoms of meningitis?
The classic triad of symptoms of meningitis in adults fever, headache, and altered mental state.

The onset may be abrupt in patients with bacterial meningitis while it may be very insidious as in patients with tuberculous and fungal meningitis.
Fever in patients with bacterial meningitis may be the very high grade that does not respond to acetaminophen or ibuprofen.
It may be temporarily relieved by cold sponges or antipyretics. Infections like tuberculosis and fungal infections may present with a low to high-grade fever, but fever is not the major complaint in these patients.

Headache may be diffuse in nature, associated with neck pain, nuchal rigidity, and stiffness.
Headache may sometimes get worse in the supine or lying position and worsens with coughing and straining.
A Headache that worsens with straining, is present or get worse after lying and resting and is associated with vomiting is an indicator of a raised intracranial pressure.
The severity of the pain again depends on the virulence of the organisms and associated complications like hydrocephalus.
Patients may also develop an altered mental status that may be noticed initially with symptoms of excessive somnolence that progress to drowsiness and coma.
Other important associated clinical features include seizures, focal weakness, problems with vision or double vision, and hearing difficulty.
Important clinical signs of meningitis include:
Neck rigidity:
- It is the resistance of the neck to passive movements and is a cardinal sign of meningeal irritation. Other classical signs of meningeal irritation are the Kernings and Bruduzinski signs.
Kernigs sign:
- It is elicited by flexing the thigh on the abdomen while the patient is lying in a supine position. Passive extension of the knee elicits pain when meningeal irritation is present.
Brudzinski’s Sign:
- Brudzinski’s sign is labeled as positive when passive flexion of the neck while the patient is lying supine, results in spontaneous flexion of the hips and knees.
Fundus examination:
- It is an important part of the examination that is done to look for papilledema. Papilledema is the blurring of the disc margins as a result of a raised intracranial pressure. Other features of a raised intracranial pressure are bradycardia and hypertension.
Specific investigations for the diagnosis of meningitis are:
- CSF examination:
- CSF examination is done by obtaining cerebrospinal fluid via lumbar puncture.
- The normal CSF has the following features:
- It is clear & Colorless
- CSF pressure of 60 to 250 mmH2o
- Up to 5 Red blood cells and 5 White blood cells in the CSF are considered normal
- The CSF protein concentration ranges from 23 to 38 mg/dl (up to 45 mg/dl is considered normal)
- The normal CSF glucose is up to 2/3rds of the serum CSF (usually greater than 45 mg/dl).
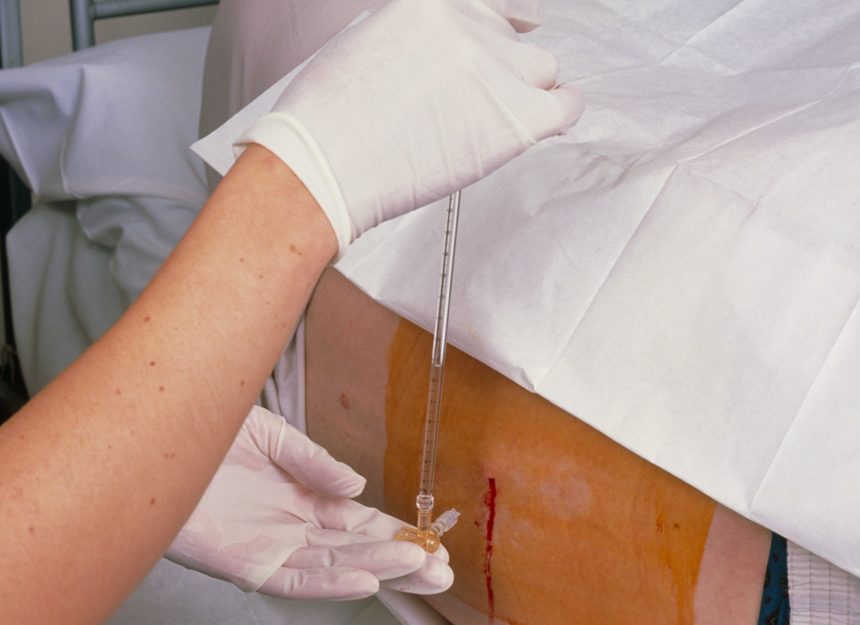
How to perform Lumbar puncture?
CSF examination may give a clue regarding the etiology of meningitis.
- CSF color:
- Clear: viral infection
- Cloudy or turbid CSF: bacterial, tuberculous, and fungal meningitis
- CSF cell counts:
- Up to 300 cells (lymphocytes dominant): viral and tuberculous meningitis
- More than 300 cells (neutrophilic predominance): Bacterial meningitis
- CSF Proteins:
- Up to 100 mg/dl: viral infection
- More than 100 ( usually more than 250 mg//dl): Bacterial infection
- More than 500 (occasionally more than 1000 mg/dl): Tuberculous meningitis
- CSF Glucose:
- Normal: viral
- Reduced in bacterial and markedly reduced in tuberculous meningitis
- CSF color:
Imaging of the brain:
A simple non-contrast CT may be advised before performing CSF examination. Patients without significant edema, an SOL especially in the occipital and cerebellar area and a normal looking fourth ventricle can safely undergo a lumbar puncture procedure.
Contrast-enhanced CT may reveal meningeal enhancement, brain abscess, and tuberculomas.
Non-diagnostic CT may be further evaluated via MR scans.